The Centers for Medicare and Medicaid (CMS) sets reimbursement rates for all medical services and equipment covered under Medicare. When a provider accepts assignment, they agree to accept Medicare-established fees. Providers cannot bill you for the difference between their normal rate and Medicare set fees.
How does the reimbursement process work?
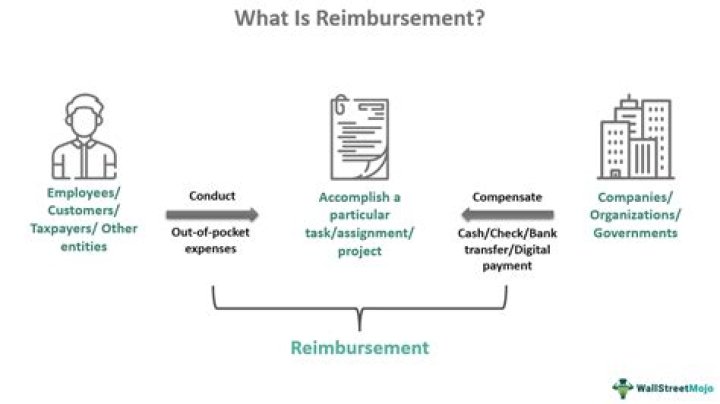
Healthcare providers are paid by insurance or government payers through a system of reimbursement. After you receive a medical service, your provider sends a bill to whoever is responsible for covering your medical costs. … Private insurance companies negotiate their own reimbursement rates with providers and hospitals.
How are Medicare reimbursements calculated?
The Centers for Medicare and Medicaid Services (CMS) determines the final relative value unit (RVU) for each code, which is then multiplied by the annual conversion factor (a dollar amount) to yield the national average fee. Rates are adjusted according to geographic indices based on provider locality.
What is the role of CMS in reimbursement?
The Centers for Medicare & Medicaid Services is a federal agency that administers the nation’s major healthcare programs including Medicare, Medicaid, and CHIP. It collects and analyzes data, produces research reports, and works to eliminate instances of fraud and abuse within the healthcare system.Does CMS reimburse on a fee for service basis?
This comprehensive listing of fee maximums is used to reimburse a physician and/or other providers on a fee-for-service basis. CMS develops fee schedules for physicians, ambulance services, clinical laboratory services, and durable medical equipment, prosthetics, orthotics, and supplies.
What is healthcare reimbursement?
A healthcare reimbursement plan, sometimes called a health reimbursement arrangement, is a health benefit where employees are reimbursed by their company for their medical expenses.
How do I claim medical reimbursement?
How to claim Medical reimbursement? One can claim reimbursement of medical expenses by submitting the original bills to the employer. The employer would accordingly reimburse such expenses incurred subject to the overall limit of Rs 15,000 without tax deduction.
What is the role of CMS in healthcare?
The Centers for Medicare and Medicaid Services (CMS) is the U.S. federal agency that works with state governments to manage the Medicare program, and administer Medicaid and the Children’s Health Insurance program. … It has summary information about health care expenses and use.What is CMS Interoperability rule?
The CMS interoperability rule requires all states to participate in daily exchange of buy-in data, which includes sending data to CMS and receiving responses from CMS. Additionally, all states must submit the MMA file data to CMS daily by April 1, 2022. This data identifies all dually eligible individuals.
Is CMS part of HHS?The Centers for Medicare & Medicaid Services, CMS, is part of the Department of Health and Human Services (HHS).
Article first time published onWhat is the Medicare reimbursement rate for nurse practitioners?
Medicare reimburses NPs at a rate of 85% of the physician fee, as stated in Medicare’s Physician Fee Schedule. So, Medicare pays the NP 80% of the 85% of the Physician Fee Schedule rate for a procedure. The total amount that the practice receives is the Medicare payment plus the patient’s payment.
What is a fee for service facility CMS?
A method in which doctors and other health care providers are paid for each service performed.
How do you calculate insurance reimbursement?
Take a look at your contract with insurance company. This contract will include the rates you’ll be reimbursed. (Usually, this is at the bottom of your contract, but each will vary.) You may decide to record them someplace easy and accessible.
Who is eligible for Medicare reimbursement?
How do I know if I am eligible for Part B reimbursement? You must be a retired member or qualified survivor who is receiving a pension and enrolled in both Medicare Parts A and B. 2.
Is an HRA use it or lose it?
In general, HRAs have no “use-it-or-lose it” policy. The employer can specify at the beginning of the year whether funds remaining in a participant’s HRA are either forfeited at the end of the plan year or whether funds can roll over and remain in the account from year to year.
Can you withdraw money from HRA?
You can’t cash out your HRA. Unused HRA funds are either rolled over to be available for eligible expenses the following year or retained by your employer — and your employer can decide which of these options to allow. But you can never choose to withdrawal HRA money for unapproved use.
What is healthcare interoperability?
Interoperability is the ability of two or more systems to exchange health information and use the information once it is received. … HHS is seeking out opportunities to accelerate and promote the development of interoperability across the health care system.
What is Medicare interoperability?
Beginning in 2011, the Promoting Interoperability (formerly the Medicare and Medicaid EHR Incentive Programs) were developed to encourage eligible professionals (EPs) and eligible hospitals and critical access hospitals (CAHs) to adopt, implement, upgrade (AIU), and demonstrate meaningful use of certified electronic …
What is interoperability and why is it important?
Interoperability ensures that patient data is shared accurately among providers and organizations, improving efficiency, decreasing unnecessary diagnostic testing, and improving communication between referring doctors and specialists.
Is CMS legitimate?
The Centers for Medicare & Medicaid Services (CMS), is a federal agency within the United States Department of Health and Human Services (HHS) that administers the Medicare program and works in partnership with state governments to administer Medicaid, the Children’s Health Insurance Program (CHIP), and health …
How do I contact CMS with questions?
- Medicare Service Center: 800-MEDICARE (800-633-4227)
- Medicare Service Center TTY: 877-486-2048.
- Report Medicare Fraud & Abuse: 800-HHS-TIPS (1-800-447-8477)
- Medicare.gov.
- Medicare Helpful Contacts Page.
- Medicare Fraud & Abuse.
What is the mission statement of CMS?
CMS’s mission is to serve Medicare & Medicaid beneficiaries. The CMS vision is to become the most energized, efficient, customer friendly Agency in the government. CMS will strengthen the health care services & information available to Medicare & Medicaid beneficiaries & the health care providers who serve them.
Is Assistant Secretary of health a cabinet position?
Assistant Secretary for HealthWebsiteOfficial website
What is the difference between the FDA and CMS?
Although FDA and CMS regulate different aspects of health care—FDA regulates the marketing and use of medical products, whereas CMS regulates reimbursement for healthcare products and services for two of the largest healthcare programs in the country (Medicare and Medicaid)—both agencies share a critical interest in …
What does a survey by CMS mean?
CMS surveys are typically conducted by the surveyors from the state department of community health and focus much more closely on patient care documentation and the corresponding policies and procedures that drive care implementation. … Typically, they spend less time on the patient care units than TJC surveyors do.
How do Nurse Practitioners Bill Medicare?
To bill Medicare for NP services (other than “incident to” services), the NP needs a performing provider number, which you can get from your Medicare carrier. NPs are allowed either to bill Medicare directly under their own provider numbers or to reassign their billing rights to employers or other contracting entities.
Can a nurse practitioner bill a 99214?
Yes, NPs can bill for 99214 and 99215 visits with the following caution: Beware in states where the scope of NP practice is not specifically defined to include comprehensive evaluations.
How are nurse practitioners reimbursed in California?
Reimbursement for services rendered by an NP can be made only to the employing physician, organized outpatient clinic or hospital outpatient department. Payment is made at the lesser of the amount billed or 100 percent of the amount payable to a physician for the same service.
Is fee-for-service good?
Economists argue that fee-for-service is inefficient and incentivizes providers to do more (tests, procedures, visits) than necessary to increase revenue. … Population health experts argue that fee-for-service payments fail to account for the low-cost but necessary care to manage chronic diseases.
Does Medicare still use fee-for-service?
Fee-for-service is a system of health care payment in which a provider is paid separately for each particular service rendered. Original Medicare is an example of fee-for-service coverage, and there are Medicare Advantage plans that also operate on a fee-for-service basis.
What is managed fee-for-service?
Under managed care, the state pays a fee to a managed care plan for each person enrolled in the plan. In turn, the plan pays providers for all of the Medicaid services a beneficiary may require that are included in the plan’s contract with the state.