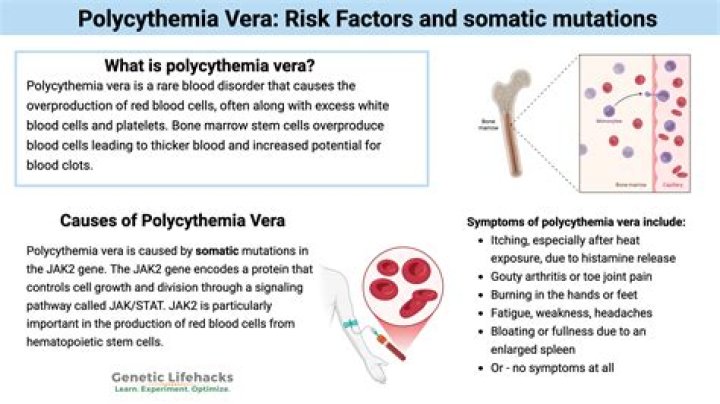
People with a new PV diagnosis typically undergo phlebotomy once a week until their red blood cell level becomes closer to normal. After that, they may have phlebotomy every three months to keep levels normal.
When is phlebotomy needed for secondary polycythemia?
Phlebotomy should be performed in any patient with secondary polycythemia prior to any elective surgery. In patients with physiologically appropriate erythrocytosis, as the increased red cell mass is a compensatory mechanism of the body, phlebotomy should not be performed in order to maintain proper tissue oxygenation.
Can Primary polycythemia be treated through phlebotomy?
The most common treatment for polychythemia vera is having frequent blood withdrawals, using a needle in a vein (phlebotomy). It’s the same procedure used for donating blood. This decreases your blood volume and reduces the number of excess blood cells.
How often can you do therapeutic phlebotomy?
Those who benefit from phlebotomy may require the procedure a few times a year or every 3 – 6 weeks. The time will vary from one person to another.What is phlebotomy as a management in polycythemia?
A phlebotomy is often the first treatment for polycythemia vera. During this therapy, your doctor removes blood from your vein. It’s a lot like donating blood. The goal is to lower the number of your blood cells.
How much blood is therapeutic phlebotomy?
Blood may be collected in a bag or in syringes. Typically, in adults, a pint of blood (450 – 500 mL) is removed at a time.
How much blood is removed in a phlebotomy?
Treatment Overview Health professionals perform phlebotomy in a medical clinic. The process is similar to donating blood. A health professional inserts a needle into a vein in your arm and removes about 500 mL (17 fl oz) of blood.
What is the most common complication of phlebotomy?
Hematoma: The most common complication of phlebotomy procedure.How much blood do you draw for polycythemia vera?
Common examples of such condi- tions are hemochromatosis and polycythemia. The proce- dure involves donation of a unit (about 500 cc) of blood on a regular basis. The blood draw stimulates the body to make new red blood cells which require iron.
What is the maximum amount of time that a tourniquet can be left on?Leaving on too long: A tourniquet should not be left for longer than two hours. When applied for a longer time, tourniquets can cause permanent damage to muscles, nerves, and blood vessels.
Article first time published onHow fast does polycythemia vera progress?
This disease develops very slowly, usually over many years. Although it can be life-threatening if you don’t get any treatment, most people have a good chance of living a long life when they get the right care. SOURCES: FamilyDoctor.org: “Polycythemia Vera.”
Can polycythemia go into remission?
A 20-year-old woman presented with polycythemia vera and was treated with phlebotomy alone for eleven years, following which all clinical manifestations of the disease disappeared. The clinical remission with normal physical findings and normal peripheral blood counts has persisted for a further 11 years.
How much does phlebotomy lower hematocrit?
The volume of phlebotomy remained a strong predictor of drop in hemoglobin and hematocrit after adjusting for other predictors using multivariate analysis (P<. 0001). On average, every 100 mL of phlebotomy was associated with a decrease in hemoglobin and hematocrit of 7.0 g/L and 1.9%, respectively.
What is the goal of phlebotomy?
The goal of phlebotomy is to lower your hematocrit level. Hematocrit is the percentage of red blood cells compared with the total amount of blood.
How much hemoglobin is too high?
The threshold for a high hemoglobin count differs slightly from one medical practice to another. It’s generally defined as more than 16.6 grams (g) of hemoglobin per deciliter (dL) of blood for men and 15 g/dL for women.
What is the latest treatment for polycythemia vera?
Today, the U.S. Food and Drug Administration approved Besremi (ropeginterferon alfa-2b-njft) injection to treat adults with polycythemia vera, a blood disease that causes the overproduction of red blood cells. The excess cells thicken the blood, slowing blood flow and increasing the chance of blood clots.
Is phlebotomy the same as giving blood?
Therapeutic phlebotomy involves the same procedure as blood donation; the primary difference is how often we give blood. Phlebotomy (aka venesection) may be recommended quite frequently for a person who has just been diagnosed with iron overload, especially if their ferritin levels are significantly elevated.
What are two conditions that cause polycythemia?
- Hypoxia from long standing (chronic) lung disease and smoking are common causes of polycythemia. …
- Chronic carbon monoxide (CO) exposure can also be a risk factor for polycythemia.
How often can you give blood?
How often can I donate blood? You must wait at least eight weeks (56 days) between donations of whole blood and 16 weeks (112 days) between Power Red donations. Whole blood donors can donate up to 6 times a year. Platelet apheresis donors may give every 7 days up to 24 times per year.
What conditions require therapeutic phlebotomy?
Therapeutic phlebotomy is currently indicated for the treatment of hemochromatosis, polycythemia vera, porphyria cutanea tarda, sickle cell disease, and nonalcoholic fatty liver disease with hyperferritinemia.
What are the side effects of phlebotomy?
Phlebotomists must follow the procedure presented in the guidelines to avoid backflow. Hematoma, allergy, hyperventilation, air embolism, anemia and thrombosis are other side effects occasionally caused by phlebotomy.
Does phlebotomy lower blood pressure?
Conclusions. In patients with METS, phlebotomy, with consecutive reduction of body iron stores, lowered BP and resulted in improvements in markers of cardiovascular risk and glycemic control. Blood donation may have beneficial effects for blood donors with METS.
Which is a late symptom of polycythemia vera?
Numbness, tingling, burning, or weakness in your hands, feet, arms or legs. A feeling of fullness soon after eating and bloating or pain in your left upper abdomen due to an enlarged spleen. Unusual bleeding, such as a nosebleed or bleeding gums.
How do you know if your blood is too thick?
The increase in blood cells makes the blood thicker. Thick blood can lead to strokes or tissue and organ damage. Symptoms include lack of energy (fatigue) or weakness, headaches, dizziness, shortness of breath, visual disturbances, nose bleeds, bleeding gums, heavy menstrual periods, and bruising.
Can a person's blood be too thick?
Blood Can Be Too Thin or Too Thick. Blood that is too thick can lead to blood clots, and blood that is too thin can lead to easy bruising or bleeding. Problems with blood thickness can occur from birth, or develop later in life. Blood thickness may be affected by foods, drugs, and various medical conditions.
What are 3 complications that can occur with a venipuncture procedure?
Complications that can arise from venepuncture include haematoma forma- tion, nerve damage, pain, haemaconcentration, extra- vasation, iatrogenic anaemia, arterial puncture, pete- chiae, allergies, fear and phobia, infection, syncope and fainting, excessive bleeding, edema and thrombus.
What needle size would not be appropriate to draw blood with?
18 Gauge Needles 18g needles are not used for routine blood draws. A needle this large is used for donating more substantial quantities of blood that require a faster blood flow rate, such as blood donor units and therapeutic phlebotomy.
Where should you not draw blood?
Do not use the tip of the finger or the center of the finger. Avoid the side of the finger where there is less soft tissue, where vessels and nerves are located, and where the bone is closer to the surface. The 2nd (index) finger tends to have thicker, callused skin.
How often should you release a tourniquet?
Periodically loosening a tourniquet For many decades, first aid classes taught that whenever a tourniquet was applied to an extremity, the tourniquet should be loosened every 15 to 20 minutes to allow blood to return into the arm or leg.
How long should a tourniquet stay on while drawing blood?
Remember that the tourniquet shouldn’t be on for more than 1 minute because it can change the blood composition. If you’re drawing multiple tubes, it’s acceptable to keep the tourniquet on when you place a new tube as long as the total tourniquet time remains less than 1 minute.
Do you keep tourniquet on when drawing blood?
Once sufficient blood has been collected, release the tourniquet BEFORE withdrawing the needle. Some guidelines suggest removing the tourniquet as soon as blood flow is established, and always before it has been in place for two minutes or more.