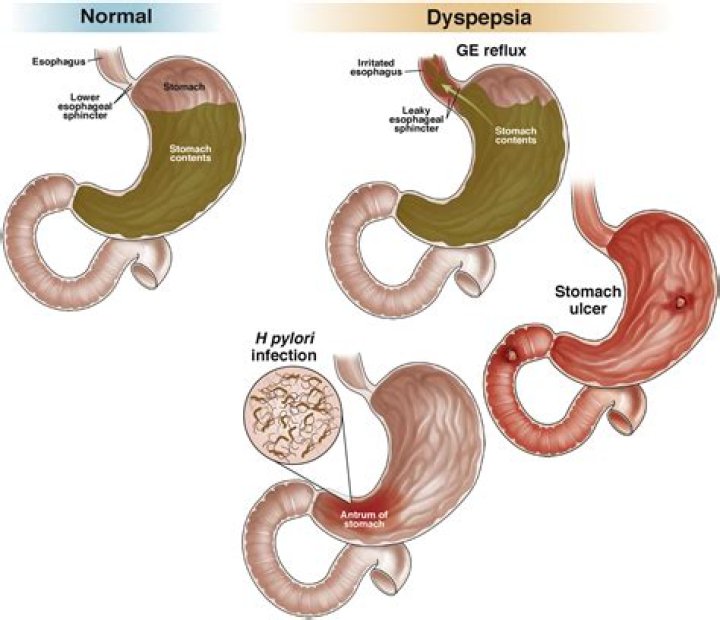
Causes of functional dyspepsia (indigestion) Functional dyspepsia is indigestion with no clear cause (such as an ulcer, gastritis or acid reflux). The gastrointestinal tract of individuals who have been diagnosed with the disorder will appear healthy.
What is the cause of functional dyspepsia?
Causes of functional dyspepsia (indigestion) Functional dyspepsia is indigestion with no clear cause (such as an ulcer, gastritis or acid reflux). The gastrointestinal tract of individuals who have been diagnosed with the disorder will appear healthy.
Can anxiety cause functional dyspepsia?
Risk factors associated with dyspepsia include Helicobacter pylori infection14, psychiatric disorders15 and behavioural factors16, while functional dyspepsia has been associated with anxiety, which sometimes precedes its onset.
How do you fix functional dyspepsia?
Functional dyspepsia is treated by two major categories of drugs: acid inhibitors such as H2-receptor antagonists and proton pump inhibitors (PPIs), and prokinetic drugs that accelerate disturbed gastrointestinal (GI) motility by modifying altered visceral sensitivity.How do you prevent functional dyspepsia?
- Over-the-counter gas remedies. …
- Medications to reduce acid production. …
- Medications that block acid ‘pumps. …
- Antibiotics. …
- Low-dose antidepressants. …
- Prokinetics. …
- Medications to relieve nausea (anti-emetics).
What foods are good for functional dyspepsia?
Rice had a good effect in 15.7% of the patients but had no effect on dyspepsia in 60% of the patients. Other nutrients like rock candy, bread, caraway seeds, dates, honey, yogurt, quinces, and walnuts were the most common foods having alleviating effects in this study (table 3).
What foods should I avoid with functional dyspepsia?
Avoid trigger foods. Some foods may trigger functional dyspepsia, such as fatty and spicy foods, carbonated beverages, caffeine, and alcohol.
How long can functional dyspepsia last?
Symptoms of functional dyspepsia Symptoms have lasted for 3 months or more and can include: Feeling full too quickly. Burping a lot. A burning feeling in the middle of your chest.Is functional dyspepsia life threatening?
Common signs and symptoms of functional dyspepsia include a burning sensation or discomfort in your upper abdomen or lower chest; bloating; belching; an early feeling of fullness when eating; and nausea. While not life-threatening, the symptoms can significantly affect your quality of life.
Does exercise help functional dyspepsia?Functional dyspepsia is associated with lower exercise levels. Reduced activity was significantly associated with functional dyspepsia, independent of age, gender, body mass index and smoking, and excluding overlap with irritable bowel syndrome .
Article first time published onWhat is the difference between dyspepsia and functional dyspepsia?
Dyspepsia is the most common upper gastrointestinal (GI) symptom, and it includes epigastric pain, fullness, discomfort, burning, early satiety, nausea, vomiting and belching. Functional dyspepsia (FD) is diagnosed when upper GI endoscopy reveals no organic lesions that might explain the dyspeptic symptoms.
How do I know if I have functional dyspepsia?
Signs and symptoms of functional dyspepsia may include: Pain or burning in the stomach, bloating, excessive belching, or nausea after meals. An early feeling of fullness (satiety) when eating. Pain in the stomach that may sometimes occur unrelated to meals or may be relieved with meals.
How do you treat functional dyspepsia naturally?
- Peppermint tea. Peppermint is more than a breath freshener. …
- Chamomile tea. Chamomile tea is known to help induce sleep and calm anxiety. …
- Apple cider vinegar. …
- Ginger. …
- Fennel seed. …
- Baking soda (sodium bicarbonate) …
- Lemon water. …
- Licorice root.
What is the difference between functional dyspepsia and GERD?
Dyspepsia is distinct from GERD and is defined as chronic or frequently recurring epigastric pain or discomfort, which is believed to originate in the gastroduodenal region. Dyspepsia may be associated with other upper gastrointestinal (GI) symptoms, such as postprandial fullness and early satiety.
Is dyspepsia the same as IBS?
[2] Many patients with IBS have dyspepsia; likewise, many patients with dyspepsia also have overlapping symptoms of IBS. These 2 groups of patients are similar in that symptoms are typically chronic in nature, may wax and wane, are aggravated by psychosocial stressors, and are often worsened by meals.
Can gluten cause functional dyspepsia?
(HealthDay)—Gluten consumption impacts symptom onset in patients with functional dyspepsia (FD), according to a study published online April 28 in the Journal of Gastroenterology and Hepatology.
Is yogurt good for dyspepsia?
Yogurt that is not too sour is also excellent for acid reflux, because of the probiotics that help normalize bowel function. Yogurt also provides protein, and soothes stomach discomfort, often providing a cooling sensation.
Can not eating cause dyspepsia?
Another scenario that often triggers dyspepsia is going too long in between meals. An empty stomach is an acidic stomach and for people with any sort of acid-related malady – from reflux to gastritis to ulcers – going more than three to four hours without eating will spell trouble.
Can you lose weight with functional dyspepsia?
The relationship between weight loss and dyspepsia has been studied and dyspepsia symptoms were found to be associated with weight loss. Nausea, vomiting, and meal-related complaints such as postprandial fullness were most strongly associated with weight loss.
Is honey good for dyspepsia?
In a clinical review published by the British Medical Journal , researchers suggested that honey’s viscous nature might help keep acids down. One member of their team saw relief from his heartburn symptoms after consuming five milliliters (about one teaspoon) of plain honey.
Is Apple good for dyspepsia?
Apples are a good source of calcium, magnesium, and potassium. It’s thought that these alkalizing minerals may help relieve symptoms of acid reflux. Acid reflux occurs when stomach acid rises into the esophagus.
What is the best medication for dyspepsia?
Examples include Alka-Seltzer, Maalox, Rolaids, Riopan, and Mylanta. These are over-the-counter (OTC) medicines that do not need a prescription. A doctor will usually recommend an antacid medication as one of the first treatments for dyspepsia.
Is functional dyspepsia hereditary?
Functional dyspepsia (FD) is a constellation of functional upper abdominal complaints with poorly elucidated pathophysiology. However, there is increasing evidence that susceptibility to FD is influenced by hereditary factors.
What does dyspepsia feel like?
Indigestion — also called dyspepsia or an upset stomach — is discomfort in your upper abdomen. Indigestion describes certain symptoms, such as abdominal pain and a feeling of fullness soon after you start eating, rather than a specific disease.
Is functional dyspepsia rare?
It affects 10% of the population and is more prevalent in women. Functional dyspepsia refers to troublesome upper gastrointestinal symptoms including inability to finish a meal (early satiety), postprandial fullness, and epigastric pain or burning.
What organs are affected by gastroparesis?
Once your stomach pulverizes the food, strong muscular contractions (peristaltic waves) push the food toward the pyloric valve, which leads to the upper portion of your small intestine (duodenum). Gastroparesis is a condition that affects the normal spontaneous movement of the muscles (motility) in your stomach.
How can I speed up gastric emptying?
- eat foods low in fat and fiber.
- eat five or six small, nutritious meals a day instead of two or three large meals.
- chew your food thoroughly.
- eat soft, well-cooked foods.
- avoid carbonated, or fizzy, beverages.
- avoid alcohol.
- drink plenty of water or liquids that contain glucose and electrolytes, such as.
Does fasting help gastroparesis?
Abdominal computed tomography, upper gastrointestinal endoscopy, and ultrasonography demonstrated gastric food retention after overnight fasting. The findings led to the diagnosis of gastroparesis. Appropriate dietary modifications alone successfully relieved the symptoms despite persistent delayed gastric emptying.
Is functional dyspepsia a symptom of GERD?
Although GERD has been linked with functional dyspepsia,23 it is evident that the likelihood of overlap between the two disorders is greater in patients with NERD than erosive disease. Within the subgroup of NERD, the overlap of functional dyspepsia is greatest among those with functional heartburn.
Can constipation cause dyspepsia?
Some patients with functional dyspepsia have also functional constipation and the investigators hypothesize that in them constipation triggers or facilitates dyspeptic symptoms, and consequently, correction of constipation relieves dyspeptic symptoms.
Is functional dyspepsia autoimmune?
Epidemiological data from the UK suggest that FGIDs are linked to atopy and certain autoimmune diseases but this has not been confirmed. Aim: To test if allergic or autoimmune diseases are independently associated with FGIDs, irrespective of psychological distress in a large population based study.