Granulocytes are sometimes measured as part of a standard complete blood count (CBC) test. The normal range of granulocytes is around 1.5 – 8.5 x 10^9/L or between 1,500 and 8,500 cells per microliter (µL) of blood.
What is a gr blood test?
Granulocytes, absolute (GR, abs) or. percentage (GR, pct) Measures the number or percentage of white blood cells with granules in. their cytoplasm and two or more lobes in their nuclei; an inclusive term.
Does immature granulocytes mean cancer?
Immature neutrophils are present in cancer and have an altered functional capacity compared to mature that may influence tumor progression. Immature neutrophils can be present and significantly increased in the peripheral blood and tissues of cancer patients.
When should I be concerned about immature granulocytes?
Immature granulocyte counts are often tests ordered for patients that are highly susceptible to develop infections. They may already have a suppressed immune system. When this test is run, if the result shows an increase, it means that the immune response will be severe.What causes Granulocytopenia?
Granulocytopenia may result from congenital or acquired defective production of granulocyte precursors or it may be a consequence of increased destruction of mature granulocytes, most frequently caused by immune mechanisms.
What is granulocyte?
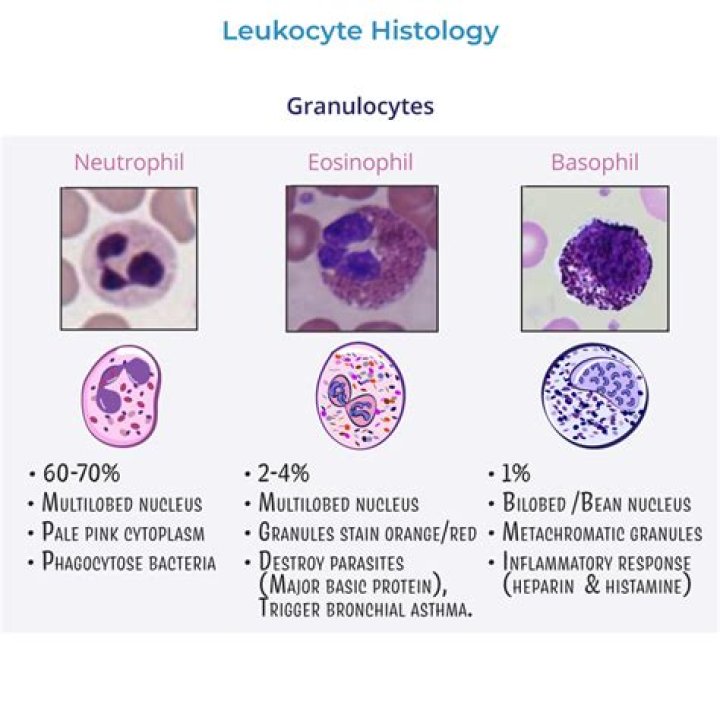
Listen to pronunciation. (GRAN-yoo-loh-SITE) A type of immune cell that has granules (small particles) with enzymes that are released during infections, allergic reactions, and asthma. Neutrophils, eosinophils, and basophils are granulocytes.
What is Nrbc in blood test?
The term ‘NRBC’ – ‘nucleated red blood cells‘ – refers to precursor cells of the red blood cell lineage which still contain a nucleus; they are also known as erythroblasts or – obsolete – normoblasts. In healthy adults and older children, NRBC can only be found in blood-building bone marrow where they mature.
Is it normal to have immature granulocytes in your blood?
Healthy individuals do not have immature granulocytes present in their peripheral blood. Therefore, the incidence of IGs in the peripheral blood is indicative of substantially increased bone marrow activation, as in different types of inflammation.Can lupus cause high immature granulocytes?
Patients with systemic lupus erythematosus (SLE) display increased numbers of immature neutrophils in the blood, but the exact role of these immature neutrophils is unclear.
What are immature white blood cells?Immature granulocytes are white blood cells that have not fully developed before being released from the bone marrow into the blood. They may include metamyelocytes, myelocytes, and promyelocytes.
Article first time published onWhy would immature neutrophils be high?
A high immature Neutrophil Count in a CBC mostly indicates the presence of infection. Neutrophils in the bone marrow go through many steps of maturation. Stem cells differentiate into successive types of immature neutrophils that end with the band form which is the final step before a fully mature neutrophil.
How do you increase your ANC count?
- colony-stimulating factors.
- corticosteroids.
- anti-thymocyte globulin.
- bone marrow or stem cell transplantation.
Are segmented neutrophils mature or immature?
Segmented or mature neutrophils have clear constrictions or segments (A). Bands (the most “mature” immature stage) have a horse-shoe shaped nucleus with no deep indentations (<50% of the width of the nucleus) (B). They can have slighter bluer cytoplasm than mature cells (more RNA).
What drugs cause Granulocytopenia?
A variety of drugs can cause acquired agranulocytosis and neutropenia by destroying special cells in the bone marrow that later mature and become granulocytes (precursors). These drugs include phenytoin, pyrimethamine, methotrexate, and cytarabine.
What are Macrocytes?
Macrocytosis is a term used to describe red blood cells that are larger than normal. Also known as megalocytosis or macrocythemia, this condition typically causes no signs or symptoms and is usually detected incidentally on routine blood tests.
What medications cause low neutrophils?
There are many medications that can result in drug-induced neutropenia. The most common are carbimazole, clozapine, dapsone, dipyrone, methimazole, penicillin G, procainamide, propylthiouracil, rituximab, sulfasalazine, and ticlopidine.
Are NRBC always bad?
Therefore, with the exception of the neonatal period, the presence of NRBCs in peripheral blood is always a pathologic finding. NRBCs may be found in the course of severe diseases and are associated with poor prognosis and higher mortality.
What is a normal NRBC count?
A normal nucleated RBC reference range for adults and children is a count of 0 nucleated RBC/100 WBC. Complete Blood Count – Everything You Need to Know. Having a count of nucleated RBC is a condition called normoblastemia. Even a count as low as 1/100 is abnormal and should be investigated.
Is NRBC bad?
Conclusions: Any positive NRBC was associated with poor outcome, and increasing NRBC was associated with increasing mortality. Trends in NRBC values showed that returning to zero was protective.
What is considered high eosinophil count?
A count of more than 500 eosinophils per microliter of blood is generally considered eosinophilia in adults. A count of more than 1,500 eosinophils per microliter of blood that lasts for several months is called hypereosinophilia.
Which white blood cells make antibodies fight infection?
Lymphocyte A lymphocyte is a type of white blood cell that is part of the immune system. There are two main types of lymphocytes: B cells and T cells. The B cells produce antibodies that are used to attack invading bacteria, viruses, and toxins.
What are the three granular white blood cells?
There are three types of granulocytes: neutrophils, eosinophils, and basophils. Each of these types is distinguished by the colour that the granules stain when treated with a compound dye. The differences in staining characteristics reflect differences in the chemical composition of the granules.
What is the most common blood disease?
Anemias, where there are not enough red blood cells or the cells do not work correctly, are among the most common blood disorders. According to the American Society of Hematology, anemia affects more than 3 million Americans.
What are the 4 types of lupus?
When people talk about lupus, they may be referring to the most common form—systemic lupus erythematosus (SLE). However, there are actually four kinds. Click or scroll to read more about each of them: SLE, cutaneous lupus, drug-induced lupus, and neonatal lupus.
Is weight gain a symptom of lupus?
Weight changes — Lupus can sometimes cause weight loss or weight gain. Weight loss may be unintentional and due to decreased appetite or problems with the digestive system (see ‘Digestive system’ below).
How high is too high neutrophils?
A normal neutrophil level is between 1,500 and 8,000 neutrophils per microliter. A high neutrophil level is over 8,000 neutrophils per microliter.
When should I be concerned about high neutrophils?
Outlook. If your neutrophil counts are high, it can mean you have an infection or are under a lot of stress. It can also be a symptom of more serious conditions. Neutropenia, or a low neutrophil count, can last for a few weeks or it can be chronic.
What is a good neutrophil count?
The number doctors look at is called your absolute neutrophil count (ANC). A healthy person has an ANC between 2,500 and 6,000.
What happens when blood count is too low for chemo?
If your blood cell levels are too low, the doctors will have to put off your next treatment until the levels have recovered. This may be called a chemotherapy break. This doesn’t matter too much. It shouldn’t make the treatment any less effective.
What happens when white blood count is too low for chemo?
This means that along with killing cancer cells, your healthy white blood cells, called neutrophils, are killed too. When the number of neutrophils is reduced, a condition called neutropenia occurs and your risk for getting an infection is increased.
What autoimmune disease causes low neutrophils?
- Crohn disease.
- Rheumatoid arthritis (with or without Felty syndrome)
- Sjögren syndrome.
- Chronic, autoimmune hepatitis.
- Hodgkin lymphoma.
- Systemic lupus erythematosus.
- Thymoma.
- Goodpasture disease.