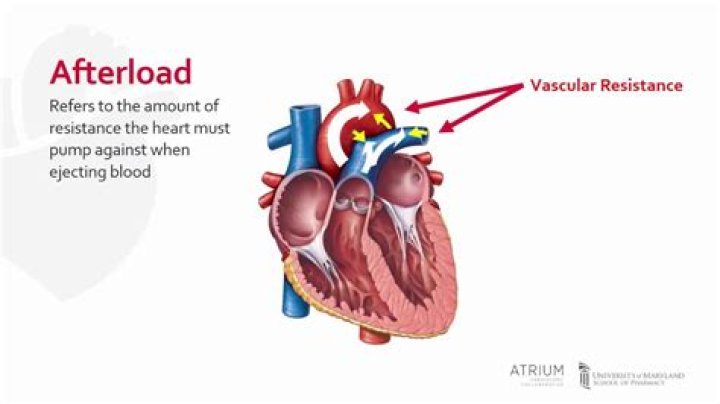
Afterload reduction agents are an essential component in treating congestive heart failure
What does afterload reduction mean?
Alteration in Afterload Pressures The lower the afterload the more blood the heart will eject with each contraction this is known as stroke volume. So you can think of this as an inverse relationship – reduced afterload = greater contraction (increased stroke volume).
What drugs are given for afterload reduction?
- Vasodilator Agents.
- Nitroprusside.
- Hydralazine.
- Nitroglycerin.
- Prazosin. Phentolamine.
What afterload means?
Afterload, also known as the systemic vascular resistance (SVR), is the amount of resistance the heart must overcome to open the aortic valve and push the blood volume out into the systemic circulation. If you think about the balloon analogy, afterload is represented by the knot at the end of the balloon.What will cause a decrease in afterload?
For example, suddenly reducing afterload by decreasing arterial pressure will lead to a reflex increase in heart rate and inotropy. Increased heart rate, by reducing filling time, will further decrease in EDV and tend to attenuate the stroke volume increase produced by reducing the afterload.
What is afterload in biology?
Afterload is the pressure that the heart must work against to eject blood during systole (ventricular contraction). Afterload is proportional to the average arterial pressure. As aortic and pulmonary pressures increase, the afterload increases on the left and right ventricles respectively.
What is afterload in the heart?
The afterload is the amount of pressure that the heart needs to exert to eject the blood during ventricular contraction. This is recorded as the systolic pressure of the heart. The changes in the afterload affect the stroke volume, end-systolic volume, end-diastolic volume, and left ventricular end-diastolic pressure.
Why is afterload important?
Because the amount of blood ejected by the ventricle, the CO, is determined largely by afterload, changes in afterload affect performance in important ways. Increased afterload causes a reciprocal decline in the extent and velocity of fiber shortening and therefore the volume of blood ejected.What happens when afterload is high?
Afterload is a measure of the force resisting the ejection of blood by the heart. Increased afterload (or aortic pressure, as is observed with chronic hypertension) results in a reduced ejection fraction and increased end-diastolic and end-systolic volumes.
How do beta blockers reduce afterload?Beta-blockers inhibit the sympathomimetic nervous system and block alpha1-adrenergic vasoconstrictor activity. These agents have moderate afterload reduction properties and cause slight preload reduction.
Article first time published onDo Calcium channel blockers lower blood pressure?
These medications lower blood pressure and treat other conditions such as chest pain and an irregular heartbeat. Calcium channel blockers are medications used to lower blood pressure. They work by preventing calcium from entering the cells of the heart and arteries.
Do diuretics reduce afterload?
Long-term treatment with diuretics may also reduce the afterload on the heart by promoting systemic vasodilation, which can lead to improved ventricular ejection. When treating heart failure with diuretics, care must be taken to not unload too much volume because this can depress cardiac output.
Does dopamine affect afterload?
Dopamine’s hemodynamic effect is dose dependent. A low dose is associated with dilation in renal and splanchnic vasculature, enhancing diuresis. Moderate doses enhance cardiac contractility and heart rate. High doses increase afterload due to peripheral vasoconstriction.
What are the effects of afterload?
Factors which affect afterload: valve resistance, vascular resistance, vascular impedance, blood viscosity, intrathoracic pressure, and the relationship of ventricular radius and volume. Determinants which are specific to the right and left ventricles.
How does a decrease in afterload affect stroke volume?
Stroke volume is reduced because increased afterload reduces the velocity of muscle fiber shortening and the velocity at which the blood is ejected (see force-velocity relationship). A reduced stroke volume at the same end-diastolic volume results in reduced ejection fraction.
Does exercise increase afterload?
The increase in arterial pressure (increased ventricular afterload) that normally occurs during exercise tends to diminish the reduction in end-systolic volume; however, the large increase in inotropy is the dominate factor affecting end-systolic volume and stroke volume.
What is normal afterload?
50 – 100 ml. Systemic Vascular Resistance (SVR) 800-1200 dynes/sec/cm5. Afterload: Afterload describes the resistance that the heart has to overcome, during every beat, to send blood into the aorta.
How do you reduce cardiac afterload?
Digitalis and diuretics constitute conventional therapy of congestive heart failure, but systemic vasodilators offer an innovative approach in acute and chronic heart failure of decreasing increased left ventricular systolic wall tension (ventricular afterload) by reducing aortic impedance and/or by reducing cardiac …
How is afterload measured?
In the clinical setting, the most sensitive measure of afterload is systemic vascular resistance (SVR) for the left ventricle and pulmonary vascular pressure (PVR) for the right ventricle. Afterload has an inverse relationship to ventricular function.
What is afterload quizlet?
Define afterload. … The afterload is the active stress that the ventricular muscle needs to generate to eject blood from the ventricle. The most common measure of afterload is the aortic pressure during ejection.
What is afterload and preload in the heart?
Preload is the initial stretching of the cardiac myocytes (muscle cells) prior to contraction. It is related to ventricular filling. Afterload is the force or load against which the heart has to contract to eject the blood.
Does increased afterload decrease blood pressure?
Increased afterload causes an increase in blood pressure. With aging, there is an increase in systolic blood pressure and a widened pulse pressure.
What is right sided heart failure?
Right-sided heart failure means your heart’s right ventricle is too weak to pump enough blood to the lungs. As a result: Blood builds up in your veins, vessels that carry blood from the body back to the heart. This buildup increases pressure in your veins.
Does digoxin decrease afterload?
2. Digoxin in increasing doses slowed the heart rate at rest; with the daily dose of 0.50 mg from 63 +/- 10 to 53 +/- 6 beats min-1, and fractional shortening rose from 28 +/- 6 to 33 +/- 3% (P less than 0.05 for both). Preload, afterload and cardiac output did not change.
Why is afterload increased in heart failure?
Hence, afterload is increased by conditions in which blood pressure and vascular tone are elevated (Table 1). Similarly, conditions that acutely elevate RV, such as acute valvular incompetence, stress cardiomyopathy or ischaemia are associated with increased afterload.
What is the most commonly prescribed beta blocker?
As seen in figure 1, the most commonly prescribed beta-blocker medications are metoprolol succinate and metoprolol tartrate. While both drugs are used to treat heart-related issues, their applications are very different.
Can I take vitamin D with calcium-channel blockers?
Similarly, normal doses of vitamin D-3 (4,000 IU a day or less) do not significantly affect calcium levels, and may be taken with calcium-channel blockers.
Is it OK to take vitamin D with amlodipine?
No interactions were found between amlodipine and Vitamin D3. This does not necessarily mean no interactions exist. Always consult your healthcare provider.
Why are calcium-channel blockers bad for you?
Calcium-channel blockers are widely used as an effective treatment for hypertension and angina. Several studies have raised questions about their safety, suggesting that calcium-channel blockers can increase the rates of myocardial infarction (MI) and death, particularly in patients with heart disease.
Does nitroglycerin decrease afterload?
The effect of nitroglycerin (NTG) is mainly a reduction in preload and afterload. The decrease in afterload may be caused by a fall of total systemic resistance (TSR) or by an increase of arterial compliance (AC). The effects of NTG on TSR and AC were tested in 10 patients given 1.6 mg NTG sublingually.
Does furosemide decrease afterload?
It reduces preload and at higher doses (> 100 mcg/min) it decreases afterload leading to increased cardiac output and decreased SVR.