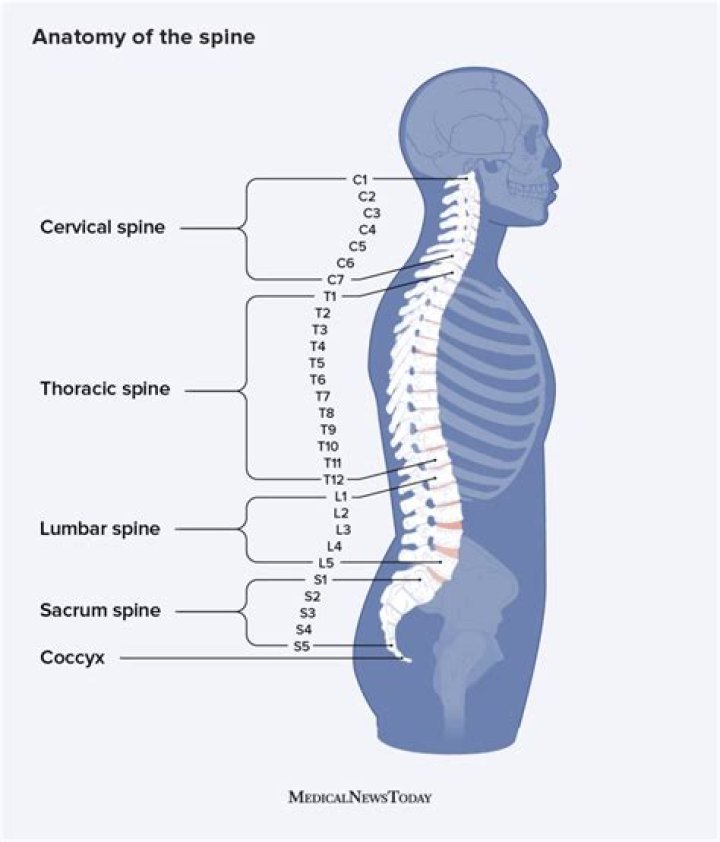
Immobilization of the cervical spine is a cornerstone of spinal injury management. In the context of suspected cervical spine injury, patients are immobilized in a ‘neutral position’ based on the head and trunk resting on a flat surface.
How do you immobilize C spine?
The traditional ATLS teaching for adequate spinal immobilization of a patient in a major trauma situation is a well fitted hard collar with blocks and tape to secure the cervical spine in addition to a backboard to protect the rest of the spine. other devices currently in use are scoop stretcher and vacuum splint.
What is spinal immobilization and why is it used?
Background: Spinal immobilisation involves the use of a number of devices and strategies to stabilise the spinal column after injury and thus prevent spinal cord damage. The practice is widely recommended and widely used in trauma patients with suspected spinal cord injury in the pre-hospital setting.
What is the purpose of C spine stabilization?
Cervical spine stabilization is a phrase applied to a variety of different techniques used in the cervical spine (the neck) to reduce or eliminate instability. Instability can be caused by degenerative disc diseases, injury, trauma, herniated discs and more.When do you use C spine precautions?
Cervical spinal precautions should be instituted immediately on suspicion of injury to immobilise the cervical spine above and below the suspected level of injury,18 preventing flexion, extension, lateral rotation and lateral flexion. A well-fitting semirigid cervical collar is adequate until imaging can be conducted.
What is manual stabilization?
Manual In-Line Stabilisation (MILS) provides a degree of stability to the cervical spine prior to the application of a cervical collar.
How do you stabilize C spine with your hands?
If the patient is awake, place both hands on either side of the patient’s head to steady it. Hold the patient’s head gently but firmly to keep it from moving. Only release the head to help with the patient’s airway, breathing, or circulation, or if the scene becomes unsafe.
Are C spine collars good?
Conclusion. Cervical collars are an accepted form of cervical immobilisation, and are prominent in the prehospital management of suspected SCI in the UK. However, recent evidence suggests that cervical collars can do more harm than good, contradicting current UK ambulance guidelines for spinal immobilisation.Do C spine collars work?
Although cervical collars can help support and protect your neck in the short-term, research has shown that long-term use of a cervical collar may lead to weakening and stiffening of your neck muscles. In cases of acute injury, this is largely unavoidable.
How do you hold C spine precautions?1. Cervical spine (c-spine) immobilization: The patient should be positioned supine in neutral alignment with no rotation or bending of the spinal column. The cervical spine should be further immobilized with use of a rigid cervical collar.
Article first time published onDoes spinal immobilization help patients?
Conclusion. Routine spinal immobilization poses no benefit to the vast majority of our patients and may indeed harm a significant number of them. The ability of paramedics to effectively clear c-spine in the field has been proven in numerous studies.
What is meant by immobilization?
: to make immobile: such as. a : to reduce or eliminate motion of (the body or a part) by mechanical means or by strict bed rest. b : to prevent freedom of movement or effective use of the planes were immobilized by bad weather. c : to withhold (money or capital) from circulation.
What is the purpose of using C spine precautions in a trauma patient?
In addition to “neck” or “C-spine precautions”, all trauma patients are cared for with thoracic and lumbar level protection. This is sometimes collectively called “C-T-L” precautions. Patients with spinal precautions are turned very carefully to prevent flexion or movement of the vertebrae.
What must you confirm before removing C collar?
The goal is to clear the C-spine within four hours. If there is a significant painful “distracting” injury, then the goal is to clear the C-spine in less than 12 hours. iii. If the CT shows abnormalities, then the orthopedic or neurosurgical spine service should be consulted prior to removing the collar.
Who needs spinal precautions?
Spinal precautions, also known as spinal immobilization and spinal motion restriction, are efforts to prevent movement of the spine in those with a risk of a spine injury. This is done as an effort to prevent injury to the spinal cord. It is estimated that 2% of people with blunt trauma will have a spine injury.
When can manual stabilization of the C spine be released?
You have established manual in-line cervical spine stabilization of an unconscious trauma patient. You may release manual stabilization: A. when the patient arrives at the hospital emergency department.
What is mils in first aid?
It is impossible to tell whether the spinal cord is permanently damaged or just temporarily squashed due to injuries to bones in the neck. MILS is the mnemonic recognised approach for protecting the head and neck in spinal trauma. … It is also known as the “trauma handshake”.
What is neurogenic shock?
Neurogenic shock is a devastating consequence of spinal cord injury (SCI). It manifests as hypotension, bradyarrhythmia, and temperature dysregulation due to peripheral vasodilatation following an injury to the spinal cord.
How do you stabilize your spine?
Different surgical procedures are used to stabilize your spine. A common surgery involves instrumentation. Your surgeon will use hardware such as facet screws, percutaneous pedicle screws, and spinous process plates to fuse the backbones together.
Are C collars still used?
Some have now replaced the rigid C-collars with a soft foam C-collar as the only device for spinal immobilization. It’s now known that current devices don’t allow for true immobilization of the spine. It’s also known that rigid C-collars cause the numerous problems as detailed in this article.
What does C collar stand for?
cervical collar (redirected from C-collar)
Why are cervical collars bad?
Finally, there is a growing body of literature showing that cervical collars are downright harmful,14 as they increase aspiration risk,15 make airway management more difficult,16 and increase intra-cranial pressure (ICP) by reducing venous return.
Why are neck collars bad?
If the collar is worn for a longer period, it could have several negative effects such as: soft tissue contractures, muscular atrophy and deconditioning, loss of proprioception, thickening of subscapular tissues and coordination, but also psychological dependence.
How long should you wear a neck collar?
A collar should not be worn for more than 10 days after a whiplash-type injury. But you may need support for a long time after surgery or traumatic injury. Emergency care is also trending away from the use of rigid collars.
Can you sit up on spinal precautions?
Have a pillow between your knees for comfort and to help maintain precautions if necessary. Tip: Change positions often and alternate rest (sitting and lying down) with activity (walking and exercise) to increase comfort. Avoid sitting and standing for long periods of time.
Can you sit up with AC collar?
You should avoid standing still or sitting for prolonged periods as this will cause your back to stiffen and your posture to deteriorate. Avoid sitting in soft low chairs as this will cause your back posture to become rounded and put added pressure on your neck.
Do you perform CPR on someone with a spinal injury?
Provide as much first aid as possible without moving the person’s head or neck. If the person shows no signs of circulation (breathing, coughing or movement), begin CPR, but do not tilt the head back to open the airway.
What is a concern while caring for the patient who is completely immobilized to a long backboard?
“The long backboard can induce pain, patient agitation, and respiratory compromise. Further, the backboard can decrease tissue perfusion at pressure points, leading to the development of pressure ulcers.”
Which of the following patients is spinal immobilization clearly indicated?
Spinal Immobilization is indicated for trauma patients where there is a suspicion of spinal injury or the patient complains of pain associated with the spinal column. Special consideration should be given when the patient age is <8 or >70 years of age.
When should a spinal board be removed?
Conclusion—The spinal board should be removed in all patients soon after arrival in accident and emergency departments, ideally after the primary survey and resuscitation phases.
What causes immobilization?
The immobilization is usually caused by spinal cord injury or extensive casting after fractures, though it can occur in settings such as Parkinson disease. Hypercalcemia after trauma requiring immobilization is common, when studied prospectively, and is usually asymptomatic.