The difference between research utilization and EBP is that research utilization may lead to changes in practice that are based on the results of one study, whereas EBP answers a clinical question based on an in-depth literature search conducted to find all relevant current research evidence related to that problem.
What are the differences between research utilization and evidence based practice?
Research utilization is the application of research findings to health care practice; EBP is considered in selecting medication options. … Research utilization is review of research publications; EBP is using the healthcare provider’s perception of what care would be best in individual situations.
What is research utilization in nursing practice?
Research utilization is the process of synthesizing, disseminating, and using research-generated knowledge to make an impact on or change in the existing nursing practice. The research utilization process was developed years ago to address the problems of using research findings in practice.
What is the relationship between research utilization Ru and evidence based practice EBP )?
What is the relationship between research utilization (RU) and evidence-based practice (EBP)? A) RU is based on an individual clinician’s personal research, while EBP is based on published research.Is research based the same as evidence based?
Science-based, Research-based, Evidence-based: What’s the difference? … Research-based – Parts or components of the program or method are based on practices demonstrated effective through Research. Evidence-based – The entire program or method has been demonstrated through Research to be effective.
What is evidence based practice in healthcare?
Evidence-based practice (EBP) is defined by Duke University Medical Center as “the integration of clinical expertise, patient values and the best research evidence into the decision-making process for patient care.”
How does nursing research relate to evidence based practice?
The inclusion of EBP in nursing provides nurses with the scientific research to make well-founded decisions. … EBP enables nurses to evaluate research so they understand the risks or effectiveness of a diagnostic test or treatments. The application of EBP enables nurses to include patients in their care plan.
What is an example of research utilization?
Digital or virtual engagement and social media can be research utilization. Knowledge management and dissemination can be research utilization. Evidence-based trainings of clinicians and the development of job aids and toolkits are also examples of this.What is the difference between best practice and evidence based practice?
Here’s the difference: Evidence-based practice is research-based practice that has been shown effective through rigorous scientific evaluation. Best practice typically does not undergo the same scientific evaluation—those processes used in research to validate the assessment or effectiveness of practice.
What is evidence-based research?Evidence-based research means that the information you use to make decisions about patient care is based on sound research, not opinion. This means you must search several sources (published articles in medical journals or in electronic form) for data, results and conclusions of valid, reputable studies.
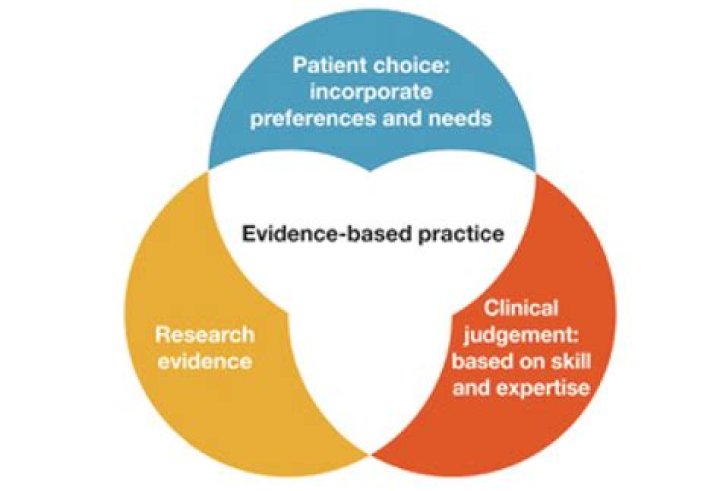
Article first time published onWhat are the 3 components of evidence-based practice?
Evidence-based practice includes the integration of best available evidence, clinical expertise, and patient values and circumstances related to patient and client management, practice management, and health policy decision-making. All three elements are equally important.
What are the steps in the research utilization process?
When research utilization is viewed as a process, five essential components emerge: (1) dissemination of research findings; (2) evaluation of scientific merit and clinical applicability; (3) incorporation of findings into practice; (4) evaluation of research-based practice; and (5) socialization into the importance and …
What's the difference between research and practice?
Research may involve introducing something non-standard or experimental to the research subjects or to the analysis of their identifiable health data. Public health practice is dominated by the use of standard, accepted, and proven interventions to address a known or suspected public health problem.
What makes a practice evidence based?
videnced-based practice (EBP) is applying or translating research findings in our daily patient care practices and clinical decision-making. EBP also involves integrating the best available evidence with clinical knowledge and expertise, while considering patients’ unique needs and personal preferences.
What is evidence based practice in nursing quizlet?
Evidence Based Practice. It is a problem-solving approach to clinical practice that combines the conscientious use of best evidence in combination with a clinician’s expertise, patient preferences and values, and available healthcare resources in making decisions about patient care.
How do nurses demonstrate evidence based practice?
- Ask: Formulate answerable clinical questions about a patient, problem, intervention, or outcome.
- Acquire: Search for relevant evidence to answer questions.
- Appraise: Determine whether or not the evidence is high-quality and valuable.
Which is the best example of evidence based nursing practice?
- Infection Control. The last thing a patient wants when going to a hospital for treatment is a hospital-acquired infection. …
- Oxygen Use in Patients with COPD. …
- Measuring Blood Pressure Noninvasively in Children. …
- Intravenous Catheter Size and Blood Administration.
What is evidence based practice and why is it important?
Why is Evidence-Based Practice Important? EBP is important because it aims to provide the most effective care that is available, with the aim of improving patient outcomes. Patients expect to receive the most effective care based on the best available evidence.
What are evidence-based practice models in nursing?
The Johns Hopkins Nursing Evidence-Based Practice Model is clinician-focused, allowing rapid and appropriate application of current research and best practices. It simplifies the EBP process and cultivates a culture of care based on evidence. It has three overall steps: practice question, evidence, and translation.
How research and evidence based practice fit together?
EBP integrates the best available research evidence with clinical expertise and patient values to improve outcomes. The process involves asking a relevant clinical question, finding the best evidence to answer it, applying the evidence to practice, and evaluating the evidence based on clinical outcomes.
Which is a major barrier to evidence based practice in nursing?
The most frequently reported organizational barriers to implementation of EBP were lack of human resources (shortage of nurse), lack of internet access at work, heavy workload, and lack of access to a rich library with nursing journals.
What strategies are framed by the utilization of evidence based medicine?
- Present solid evidence. …
- Adopt a compassionate approach. …
- Include links to information in EHR systems. …
- Use clinical decision support.
What are the different types of research reports?
- Long Report and Short Reports. …
- Internal and External Reports. …
- Vertical and Lateral Reports. …
- Periodic Reports. …
- Formal and Informal Reports. …
- Informational and Analytical Reports. …
- Proposal Reports. …
- Functional Reports.
Which goal is the highest priority for research in the nursing profession?
What is the highest priority for the importance of research in the nursing profession? –Research findings provide evidence for informing nurses’ decisions and actions.
What is quality improvement in nursing?
The definition of quality improvement (QI) is, “Using data to monitor the outcomes of care processes and using improvement methods to design and test changes to continuously improve the quality and safety of health care systems” (QSEN, 2003).
What is the main difference between research and clinical practice?
While there are a lot of similarities, the key difference is that medical treatment is intended to benefit and help you while using accepted procedures and products, whereas clinical research is intended to learn about a medication to potentially help patients in the future.
What are two primary causes of the research to practice gap?
Research‐to‐practice gaps have always existed and progress in this subject has been slow. Factors that contribute to this problem include lapses in communication between researchers and practitioners, and service delivery issues such as lack of public awareness, poor financing and a non‐supportive political atmosphere.
What is the difference between a practitioner and a researcher?
As nouns the difference between researcher and practitioner is that researcher is one who researches while practitioner is a person who practices a profession or art, especially law or medicine.