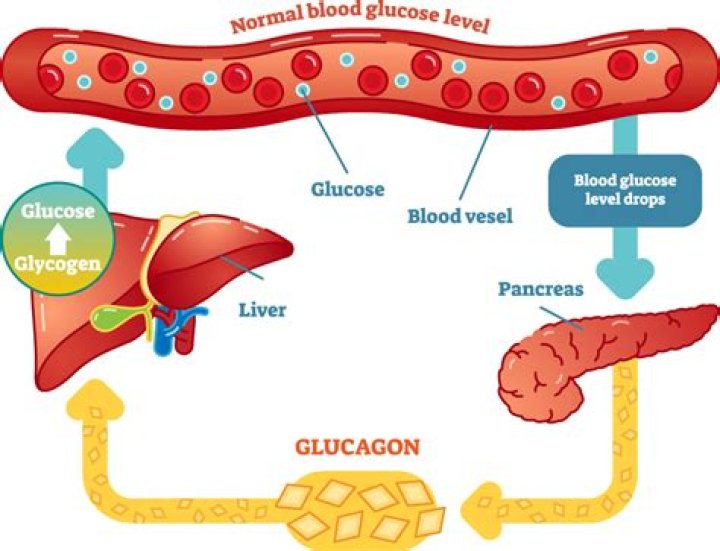
A spike in insulin signals to the liver that blood glucose is also high. The liver absorbs glucose then changes it into a storage molecule called glycogen. When blood sugar levels drop, glucagon instructs the liver to convert the glycogen back to glucose, causing blood sugar levels to return to normal.
When blood glucose levels are high the liver releases?
During a meal, your liver will store sugar, or glucose, as glycogen for a later time when your body needs it. The high levels of insulin and suppressed levels of glucagon during a meal promote the storage of glucose as glycogen.
When glucagon in the blood is high the liver will?
Glucagon exerts control over two pivotal metabolic pathways within the liver, leading that organ to dispense glucose to the rest of the body: Glucagon stimulates breakdown of glycogen stored in the liver. When blood glucose levels are high, large amounts of glucose are taken up by the liver.
Is glucagon released when blood glucose levels rise?
Glucagon is released to stop blood sugar levels dropping too low (hypoglycaemia), while insulin is released to stop blood sugar levels rising too high (hyperglycaemia). The release of glucagon is stimulated by low blood glucose, protein-rich meals and adrenaline (another important hormone for combating low glucose).Does the liver release glucagon?
Glucagon is released in response to LOW blood glucose (sugar) levels. It normalizes blood sugar levels by stimulating the release of stored glucose from the liver, by stimulating out the liver to make more glucose, and by reducing how much glucose the liver needs to function.
What occurs when blood glucose levels rise?
Normally, blood glucose levels increase after you eat a meal. When blood sugar rises, cells in the pancreas release insulin, causing the body to absorb glucose from the blood and lowering the blood sugar level to normal.
How does the liver lower blood glucose concentration when it is too high?
A spike in insulin signals to the liver that blood glucose is also high. The liver absorbs glucose then changes it into a storage molecule called glycogen. When blood sugar levels drop, glucagon instructs the liver to convert the glycogen back to glucose, causing blood sugar levels to return to normal.
What causes high glucagon levels?
The most common cause of hyperglucagonemia is an absence or deficiency of the restraining influence of insulin on glucagon production. Although rare, hyperglucagonemia can be caused by an autonomous secretion of glucagon by a tumor of pancreatic alpha cells (glucagonoma syndrome).How does glucagon travel from the pancreas to the liver?
If the blood glucose level is too low, glucagon is released by the pancreas and travels through the blood. It binds to receptors on the liver, which causes the liver to break down the stored glycogen and release glucose back into the blood.
Why does glucagon increase insulin secretion?Glucagon also activates specific G-protein coupled receptors on pancreatic β-cells leading to activation of adenylate cyclase and subsequent stimulation of insulin secretion (14).
Article first time published onHow does glucagon control blood sugar?
Glucagon works to counterbalance the actions of insulin. About four to six hours after you eat, the glucose levels in your blood decrease, triggering your pancreas to produce glucagon. This hormone signals your liver and muscle cells to change the stored glycogen back into glucose.
How does glucagon increase gluconeogenesis?
Glucagon opposes hepatic insulin action and enhances the rate of gluconeogenesis, increasing hepatic glucose output. In order to support gluconeogenesis, glucagon promotes skeletal muscle wasting to supply amino acids as gluconeogenic precursors.
How does epinephrine increase blood glucose?
When blood glucose levels drop too low, the adrenal glands secrete epinephrine (also called adrenaline), causing the liver to convert stored glycogen to glucose and release it, raising blood glucose levels.
What happens when blood glucose is too high GCSE?
If the blood glucose concentration is too high, the pancreas produces the hormone insulin that causes glucose to move from the blood into the cells. In liver and muscle cells excess glucose is converted to glycogen for storage, and will be used at a later date.
Why does the concentration of glucose in the blood decrease?
The concentration of glucose in a person’s blood can decrease after a period of exercise or if they have not eaten for a long while. Glucose diffuses out of the blood into muscle cells and is broken down to release energy for muscle contractions.
What is the role of the liver in blood glucose homeostasis?
The most important role of the liver in glucose homeostasis is to maintain a stable fast blood glucose level in the fasting state through gluconeogenesis, glycogenolysis and glycogen synthesis.
How do you reduce glucose in the liver?
One method to inhibit glucose release by the liver is to increase its storage as glycogen. In diabetic patients, hepatic glycogen synthesis is impaired83 and the stimulation of glycogen synthesis in skeletal muscle by insulin is stunted, contributing to insulin resistance84.
Does your liver release insulin?
The insulin released from the liver acts on adipose and muscle tissue to stimulate glucose uptake. These actions of insulin at the three main insulin-sensitive tissues maintain blood glucose levels within a narrow range of approximately 80−120 mg/dL.
What happens when there is too little glucagon?
That’s the fuel your muscles and organs use to work and stay healthy. Glucagon helps your liver break down the food you eat to make glucose. If your blood sugar drops too low, you can get hypoglycemia. This can make you feel dizzy or sluggish or even pass out.
How does glucose triggers insulin release?
Glucose elicits rapid insulin release through an adenosine triphosphate‐sensitive K+ channel (KATP channel)‐dependent mechanism, which is gradually augmented in a KATP channel‐independent manner. Biphasic GSIS thus occurs.
What stimulates release of insulin?
Insulin secretion is governed by the interaction of nutrients, hormones, and the autonomic nervous system. Glucose, as well as certain other sugars metabolized by islets, stimulates insulin release.
What does epinephrine do to the liver?
In the liver, epinephrine stimulates the breakdown of glycogen to glucose, resulting in an increase in glucose levels in the blood. It also acts to increase the level of circulating free fatty acids.
What is the major function of glucagon in the body?
Glucagon Increases Hepatic Glucose Production Specifically, glucagon promotes hepatic conversion of glycogen to glucose (glycogenolysis), stimulates de novo glucose synthesis (gluconeogenesis), and inhibits glucose breakdown (glycolysis) and glycogen formation (glycogenesis) (Fig.
Why is epinephrine released?
Strong emotions such as fear or anger cause epinephrine to be released into the bloodstream, which causes an increase in heart rate, muscle strength, blood pressure, and sugar metabolism. This reaction, known as the “Flight or Fight Response” prepares the body for strenuous activity.
What does the liver do in response to insulin?
Insulin stimulates the liver to store glucose in the form of glycogen. A large fraction of glucose absorbed from the small intestine is immediately taken up by hepatocytes, which convert it into the storage polymer glycogen.
What is glucagon GCSE?
Glucagon stimulates the liver to breakdown its store of glycogen into glucose, which is then released into the blood to increase the level of blood glucose.
What happens when blood glucose falls too low GCSE?
Negative feedback Whereas, if the blood glucose level is too low, the liver receives a message to release some of that stored glucose into the blood. This change is brought about by another hormone produced by the pancreas called glucagon.