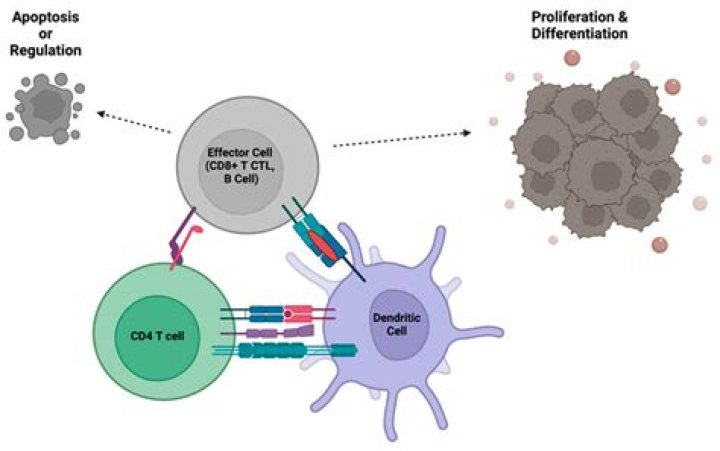
Lymphocytes are a type of white blood cell in your immune system. This test looks at two of them, CD4 and CD8. CD4 cells lead the fight against infections. CD8 cells can kill cancer cells and other invaders.
What is the role of CD4 and CD8?
Main Function of Both CD4 and CD8 Is to Enhance Lck Recruitment, Not Stabilize TCR–pMHC Interactions. Although CD4 does not stabilize TCR–pMHC interactions (9, 13, 14), like CD8, it does enhance T-cell responses (1, 9).
What is the role of CD8+ T cells?
CD8+ T cells (often called cytotoxic T lymphocytes, or CTLs) are very important for immune defence against intracellular pathogens, including viruses and bacteria, and for tumour surveillance. … This pore allows the granzymes also contained in the cytotoxic granules to enter the infected or malignant cell.
What is the main function of a CD4 T cell?
A key role of CD4+ T cells is to ensure optimal responses by other lymphocytes. CD4+ T cells are necessary as helpers to promote B cell antibody production and are often required for the generation of cytotoxic and memory CD8+ T cell populations.What is macrophage?
Listen to pronunciation. (MA-kroh-fayj) A type of white blood cell that surrounds and kills microorganisms, removes dead cells, and stimulates the action of other immune system cells.
What is the difference between NK cells and CD8 T cells?
Functionally, NK cells had increased expression of granzyme B compared to bystander-activated CD8 T cells. Thus, although NK and bystander CD8 T cells can fill a similar immunologic niche regarding target cell killing, there are significant differences in expression of critical markers following activation.
What are CD8 receptors?
CD8 (cluster of differentiation 8) is a transmembrane glycoprotein that serves as a co-receptor for the T-cell receptor (TCR). Along with the TCR, the CD8 co-receptor plays a role in T cell signaling and aiding with cytotoxic T cell antigen interactions.
Does CD4 activate CD8?
CD4 T cell activation during peripheral infections not only is essential in inducing protective CD8 T cell memory but also promotes CD8 T cell function and survival. However, the contributions of CD4 T cell help to antiviral CD8 T cell immunity during central nervous system (CNS) infection are not well established.Does CD8 need CD4?
Although the primary CD8 T cell response to infections can be independent of CD4 T cell help, recent studies have indicated that CD4 T cell help is required for the generation of long-lived, functional memory CD8 T cells that respond rapidly upon secondary exposure to pathogens (23, 24, 25).
What is the function of macrophage?Macrophages are key components of the innate immune system that reside in tissues, where they function as immune sentinels. They are uniquely equipped to sense and respond to tissue invasion by infectious microorganisms and tissue injury through various scavenger, pattern recognition and phagocytic receptors1,2,3,4.
Article first time published onWhat are macrophages function?
Macrophages are tissue-resident or infiltrated immune cells critical for innate immunity, normal tissue development, homeostasis, and repair of damaged tissue. Macrophage function is a sum of their ontogeny, the local environment in which they reside, and the type of injuries or pathogen to which they are exposed.
What is peritoneal macrophage?
Peritoneal macrophages are the macrophages that reside in the peritoneal cavity, a fluid-filled space located between the wall of the abdomen and the organs found in the abdomen. In the absence of peritoneal infection or inflammation, peritoneal macrophages are thought to have anti-inflammatory functions.
How do CD4 cells help CD8 cells?
CD4+ T cells regulate the secondary responsiveness of CD8+ T cells during immunization through suppression of TNF-related apoptosis-inducing ligand (TRAIL) through a process dependent on licensing of DCs to produce interleukin-15 (IL-15) and autocrine secretion of IL-2 by CD8+ T cells.
How do CD4 cells activate CD8 cells?
CD40–CD40L signaling pathway In this model, the CD40L expressing CD4 T cells can interact with the professional APC-DC through the CD40–CD40L pathway. This interaction can lead to the activation/licensing of DC, then the licensed DC can activate CD8 CTL cells.
What cells express CD4?
CD4 is normally expressed on helper T cells, where it plays an important role in the recognition of MHC molecules on the surface of adjacent cells. However, it can also be expressed on many other hemopoietic cell types, including macrophages, eosinophils, neutrophils, and CD8+ T cells (8, 9, 10, 11, 12, 13).
Do NK cells express CD4 or CD8?
Type I NKT cells constitutively express various T cell markers such as the TCR signaling complex CD3, and costimulatory receptors such as CD4, CD8, and CD28 (27–31).
Does natural killer cells have CD8?
Cytotoxic T-lymphocytes co-express the T-cell receptor, CD3 and the MHC I restricted antigen CD8. Although total CD8 expression is often used to identify CD8(+) T-cells in blood, errors are associated with this method as some CD3 negative natural killer (NK)-cells are known to express CD8.
Are NK cells CD8 positive?
The majority are CD8+ and they variably express NK-cell–associated antigens, including CD56 and CD57.
Do CD8 T cells secrete cytokines?
CD8+ T cells mediate their effector functions through production of cytokines such as IFN-γ and tumor necrosis factor (TNF)-α and/or by cytolytic mechanisms.
What are the functions of fibroblasts macrophages and mast cells?
Fibroblasts are responsible for the synthesis and the degradation of fibrous and non fibrous connective tissue matrix proteins. Macrophages are phagocytic; they process and present antigen to immunocompetent lymphoid cells. Mast cells are responsible for IgE mediated acute, subacute and chronic inflammation.
What is the function of macrophages in connective tissue?
Macrophages. Macrophages are phagocytic cells that engulf and digest microbes, cellular debris, and foreign substances. Monocytes develop in bone marrow, circulate in the bloodstream, and migrate into connective tissue, where they differentiate into macrophages.
What is the role of the macrophage during antibody formation?
One of the most important functions performed by macrophages during the induction of an immune response may be the presentation of antigen to antibody-forming cell precursors in a molecular form appropriate for cell activation.
What is the function of monocytes?
A type of immune cell that is made in the bone marrow and travels through the blood to tissues in the body where it becomes a macrophage or a dendritic cell. Macrophages surround and kill microorganisms, ingest foreign material, remove dead cells, and boost immune responses.
What are the function of lymphocytes?
Lymphocytes are white blood cells uniform in appearance but varied in function and include T, B, and natural killer cells. These cells are responsible for antibody production, direct cell-mediated killing of virus-infected and tumor cells, and regulation of the immune response.
What is the function of B lymphocytes?
B lymphocytes play a critical role in pathogen-specific immunity by producing antibodies. B lymphocytes recognize soluble antigens via immunoglobulins anchored on their surface and differentiate into antibody-producing cells, called plasma cells, capable of secreting immunoglobulins.
What is peritoneal lining?
The peritoneum is the serous membrane forming the lining of the abdominal cavity or coelom in amniotes and some invertebrates, such as annelids. It covers most of the intra-abdominal (or coelomic) organs, and is composed of a layer of mesothelium supported by a thin layer of connective tissue.
What are peritoneal cells?
Abstract. The peritoneal cavity is a membrane-bound and fluid-filled abdominal cavity of mammals, which contains the liver, spleen, most of the gastro-intestinal tract and other viscera. It harbors a number of immune cells including macrophages, B cells and T cells.
How are macrophages produced?
Macrophages are formed through the differentiation of monocytes, one of the major groups of white blood cells of the immune system. When there is tissue damage or infection, the monocytes leave the bloodstream and enter the affected tissue or organ and undergo a series of changes to become macrophages.
What is the difference between CD4 and CD8 T cells?
The main difference between CD4 and CD8 T cells is that the CD4 T cells are the helper T cells, which assist other blood cells to produce an immune response, whereas the CD8 T cells are the cytotoxic T cells that induce cell death either by lysis or apoptosis.
What does CD4 stand for?
In molecular biology, CD4 (cluster of differentiation 4) is a glycoprotein that serves as a co-receptor for the T-cell receptor (TCR). CD4 is found on the surface of immune cells such as T helper cells, monocytes, macrophages, and dendritic cells.
What is CD4 help in the contest of CD8 T cell memory CD4 help is necessary?
CD4+ T cell help is required for DCs to increase their antigen-presentation and co-stimulatory capacity to levels sufficient to induce a robust effector CD8+ T cell response, with both the CD4+ and CD8+ T cells recognizing antigen presented by the same DC 22.